The birth of your baby (whether at home, at a hospital, or at a birth center) is not regulated by the US government, but by individual states. In Texas, out-of-hospital (OOH) births are almost exclusively performed by midwives. The majority of these midwives are Licensed Midwives, and some are Certified Nurse Midwives. Physicians will be discussed because information about their regulation is useful for comparison. At this time, physician-attended home birth is very rare in Texas, if it happens at all. The differences in training between these practitioners can be found on the PROVIDERS page. This page will cover the legal regulation of these delivery attendants and of the practice of OOH birth in Texas. Licensed Midwives (non-nurse midwives) will be emphasized because they are the predominant providers of out-of-hospital birth. The state has regulated midwifery practice since the Texas Midwifery Act was passed in 1983.
In some states, midwifery is still unregulated. This means that simply anyone is allowed to advertise as a “traditional midwife” and deliver babies. Due to higher safety standards in our state, that type of practice has been eliminated here.

The International Confederation of Midwives is a non-governmental organization made up of midwifery organizations around the globe. The Confederation has collaborated with the World Health Organization to develop the International Definition of a Midwife and has established Global Standards for midwifery education and regulation as well as Essential Competencies for the practice of midwifery. Midwives in the US have organized to form the Midwives Alliance of North America, which participates in the International Confederation. MANA conducts research and advocates for practice rights on behalf of direct-entry midwives across the US.
The State of Texas looks to MANA (which coordinates with the ICM) to define what midwifery is, and what makes a midwife competent to perform her job. The State then uses that information, combined with available evidence, to regulate the practice of midwives in the state.
To make sure we understand how regulation works, let’s first discuss licensure versus certification.
Licensure is a state’s grant of legal authority to practice a profession within a designated scope of practice. It is a mandatory process to legally perform certain jobs, such as a license to repair elevators, provide beauty services (cosmetology), or to practice medicine.
Certification is usually a voluntary process administered by a private, academic, or professional organization for the purpose of informing the public that those individuals who are credentialed can perform their duties competently. For example, board certification in a certain specialty (like OB/Gyn or Family Medicine) for a physician. Certification is sometimes required before a state will grant licensure in a given profession.
Licensure and Certification both exist to protect and inform the public. This system is designed so that the public can differentiate between who is trustworthy, and who might be dangerous or trying to take advantage of them. In Texas, physicians and CNMs who deliver babies are required to be certified by their respective professional organization and then licensed by the state. Non-nurse midwives are required to be licensed, but they are not required to be certified.
Now, let’s explore how providers who deliver Texas babies are licensed, certified, and regulated.
Physicians are certified by their respective specialty Board of the American Board of Medical Specialties, the American Osteopathic Association, or the American Board of Physician Specialties. These certifying organizations require that the doctor has completed all the necessary education, exams, and has obtained the necessary training and experience to be competent in their field. Any physician delivering any woman’s baby in Texas should be board certified. Physicians are licensed and regulated by the Texas Medical Board.
Certified Nurse Midwives are certified by the American Midwifery Certification Board. They are then licensed and regulated by the Texas State Board of Nursing.
Direct-Entry Midwives are often certified by the North American Registry of Midwives, which awards the Certified Professional Midwife (CPM) credential. Unlike the above professions, there are several pathways to obtain the CPM certification, which require different levels of training. In Texas, it is still possible to become a Licensed Midwife without being certified as a CPM. These pathways are discussed on the PROVIDERS page.
To practice midwifery in Texas, an individual must hold a current license issued by the Texas Department of Licensing and Regulation (TDLR). This program applies only to direct-entry midwives, sometimes called lay-midwives because their practice and licensure do not require formal undergraduate or graduate education.
Direct-entry midwives were previously regulated by the Texas Department of State HealthServices, but in 2016 transitioned along with several other health professions to the Texas Department of Licensing and Regulation (TDLR).

This is the same government entity that regulates plumbers, cosmetologists, elevator repairmen and tow truck operators. The Midwives Program of TDLR oversees their practice and their approved education courses in the state.
It is important to note that it’s possible for any provider, including a direct-entry midwife to be certified but NOT licensed. Simply holding a credential does not mean any provider can legally deliver babies in Texas. If a provider is employed by a health system or other organization, you can be more certain that they will have a current license. If your provider is independent, as many direct-entry midwives are, a prospective client should verify that her midwife has a current license. You can find out if a midwife is licensed by visiting the TDLR Midwives License file, which is updated daily. Just click this link and under “Health Professions” choose “Midwives” to download the current file. There are around 240 licensed midwives practicing in Texas as of February 2018.
Be very careful if considering delivering your baby with any unlicensed practitioner. Not only is their practice unlawful, there may be important reasons why they were denied a license or why their license was removed or suspended, such as criminal activity, malpractice, or ongoing investigation.
It is important to be aware of that in Texas:
- Practicing medicine without a license is a felony
- Practicing nursing without a license is a felony
- Practicing midwifery without a license currently carries no civil or criminal penalty as of September 2017.
- Without severe penalties to prevent fraud, potential clients should be especially careful to choose a licensed provider
Other providers:
The above providers (Physicians, CNMs, and LMs) are the ONLY providers legally permitted to deliver babies in Texas. Other types of midwives exist, such as Certified Midwives, traditional midwives, and parteras, which are explained on the PROVIDERS page. These providers are not licensed by the State of Texas and are not permitted to legally practice here.

What if something goes wrong at my birth?
Childbirth, while a natural process, carries risk. There is risk in the process of childbirth that is completely unavoidable. There is also avoidable risk in the process due to human error. This section will explore those human factors and what protections exist for the public surrounding birth attendant malpractice.
Again, we’ll address each provider individually. The hypothetical scenario is the injury or death of mother or baby during labor and delivery. We will mostly discuss the legal consequences of an adverse event during a Texas birth, and what type of accountability exists for these providers. Differences in the types of medical crises or adverse events that different providers are trained to manage are discussed on the PROVIDERS page.
For Physicians:
If there is an adverse outcome in a hospital such as the death of a child, an internal review of the case by a team of physicians and other professionals is immediately triggered. Peer review can include evaluating the merits of a complaint regarding a practitioner, the accuracy of a diagnosis, the quality of care provided, or the qualifications of a practitioner. This review happens as rapidly as possible.
This peer review process may or may not lead to a complaint being placed with the Texas Medical Board. The Board will review the case to determine whether the physician was not delivering the standard of care or may have violated the Medical Practice Act. You can look up any physician’s license history and record of violations on the TMB website here.
Independent of the Board review process, a malpractice lawsuit may be filed against the physician in question. Any Texas physician employed by a health system or other entity carries malpractice insurance, which will be discussed below.
Certified Nurse Midwives who practice in hospitals are subject to the same type of institutional peer-review as employed physicians. This may not be the case for CNMs who practice in freestanding birth centers. In the out-of-hospital context, the case review and discipline process would begin with a complaint to the Texas Board of Nursing. A list of violations and sanctions for nurses can be found in the Nursing Practice Act. This video explains the process of filing a complaint to case resolution for nurses in Texas, including nurse midwives. You can verify a nurse’s license and see violation history here.
Licensed Midwives
Because Licensed Midwives are are not permitted to practice in Texas hospitals, they are exclusively independent practitioners. This means there is no automatic institutional peer review process that would occur after an adverse event. A case review or discipline proceeding would only be triggered by the filing of a complaint to TDLR. The client or her partner may be the only person besides the midwife who was present at her birth. For this reason, it is important for a client to know what a Licensed Midwife is and is not allowed to do based on Texas statute and rules. These are discussed on the STANDARDS OF CARE page. A list of violations and corresponding sanctions for Texas LMs can be found here.
Licensed Midwives who choose to attain or maintain the Certified Professional Midwife (CPM) credential are required to participate in five hours of community peer review with other independent midwives every three years or attend a one-day peer-review workshop. Not all Licensed Midwives in Texas ever attain or maintain the CPM credential.
The National Practitioner Data Bank
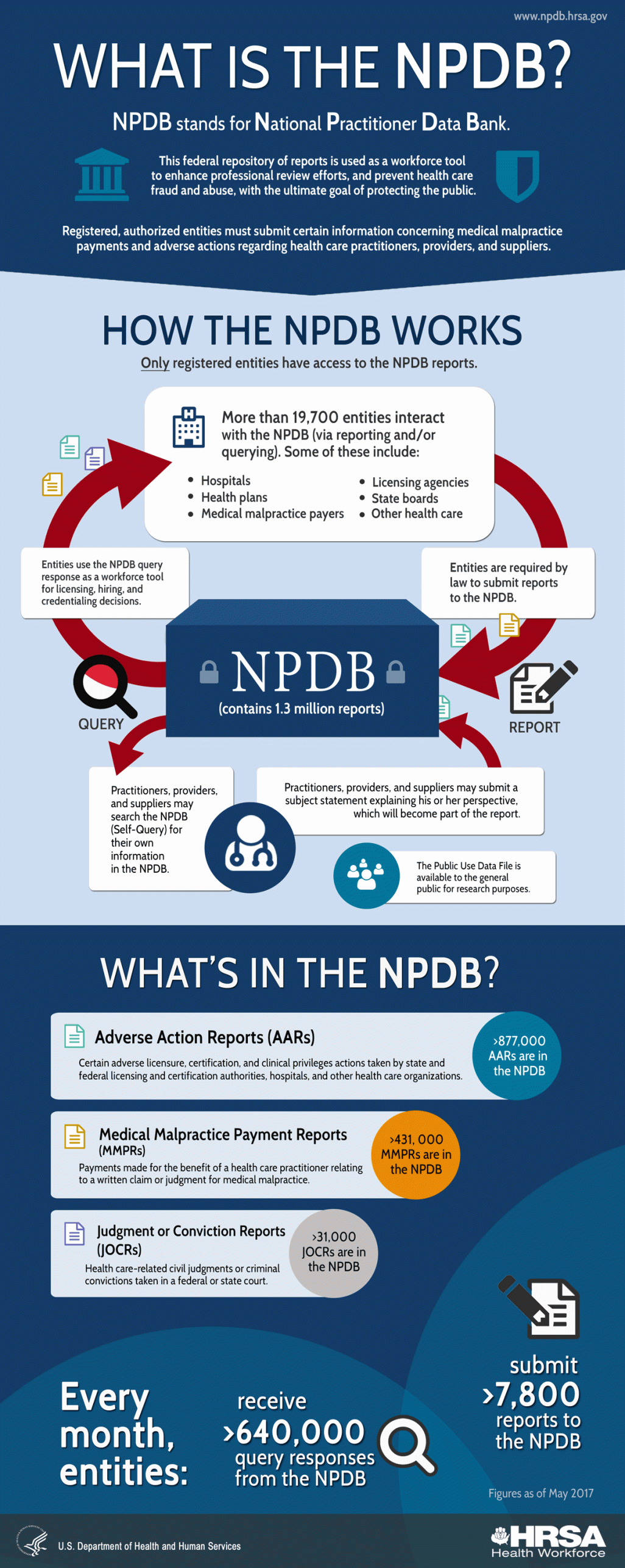
The Health Care Quality Improvement Act of 1986 protects the public nationwide by making sure that physicians and other providers cannot move to another state and practice without disclosing their malpractice violations and license violations. The Act established the National Practitioner Data Bank, which tracks adverse actions, judgments, and malpractice cases nationally. This database includes many different types of healthcare service providers, including physicians, CNMs, and direct-entry midwives.
It should be noted that in Texas, offenses by physicians and nurse midwives are reported to the NPDB. Offenses by direct-entry midwives are not reported. This means that a midwife could have license violations or malpractice judgments in her history that would not follow her and would not prevent her from practicing in another state.
Malpractice Insurance
Delivering babies is a human endeavor. Humans make mistakes, and therefore human error is part of the process.
Many types of healthcare providers carry malpractice insurance. The purpose of this insurance is to make certain that, in the event of injury or death that results from error by the provider, the patient/client will receive adequate compensation. The State of Texas does not require that physicians, nurses, or midwives carry malpractice insurance. However, all accredited hospitals and health systems require employed providers to carry insurance. As with licensure, independent providers may differ, and may not carry malpractice insurance. This can have an impact on your delivery.
Choosing any type of provider to deliver your baby who does not have malpractice insurance means that you may have difficulty getting compensation if something goes wrong. In a malpractice case, the provider’s insurance pays for the plaintiff’s attorney fees and court costs. These are frequently thousands of dollars. If your provider is uninsured, you’ll be paying that money yourself. Additionally, a provider without malpractice insurance can declare bankruptcy to avoid paying compensation fees to a client/patient. These are just a few important topics to consider when deciding on a provider. You can read more about these risks here and here.